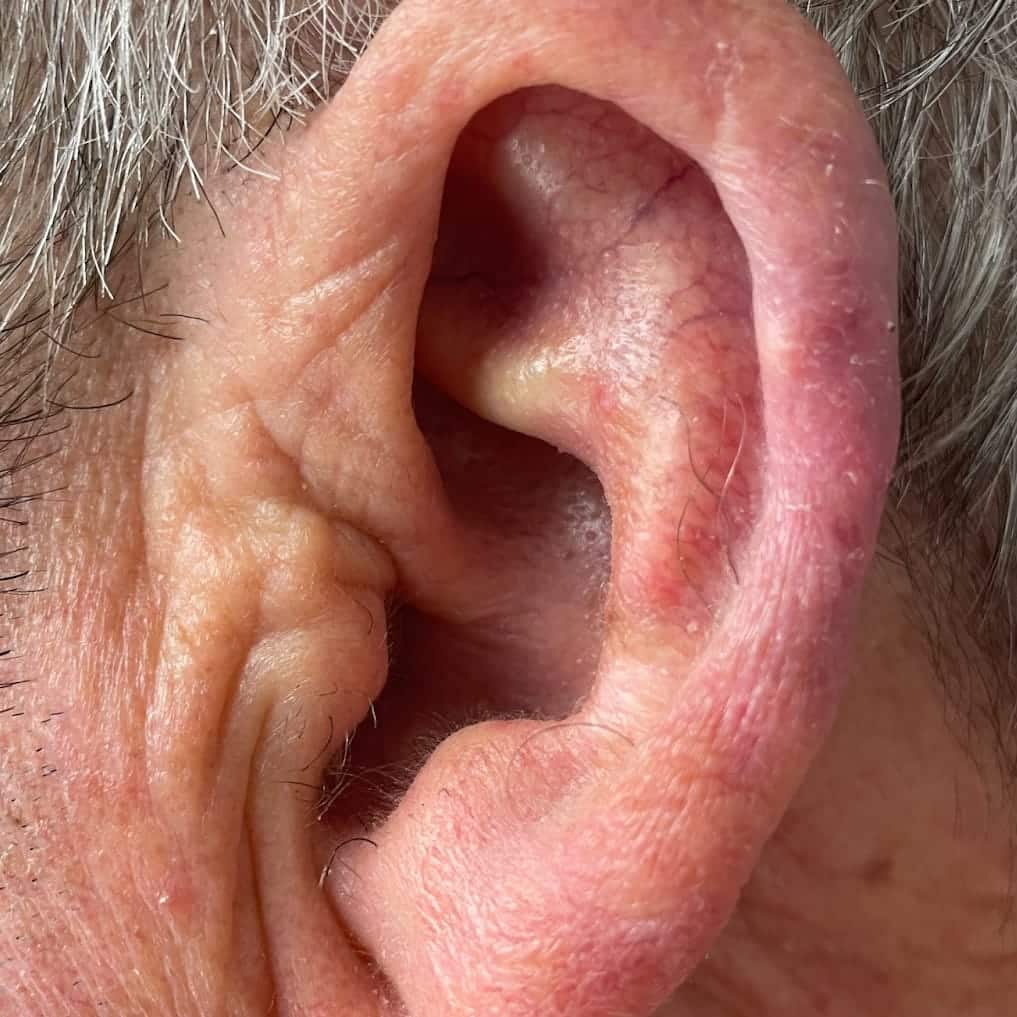
Itching. Burning. Water intolerance. Joint pain. These are only a few of the symptoms that you may experience with psoriasis on the hands and feet if you have the variant with pustules. This first visit may be years after you have noticed your first pustule, your treatment delayed due to the embarrassment and psychological distress you feel by having a rash in such a visible location.
What to do if you have pustular psoriasis
So you think that your rash could be psoriasis with pustules. What next? Here are a few steps we recommend you take if you suspect you have pustular psoriasis.
1. Cut down on smoking.
Smoking is perhaps the most common trigger of psoriasis with pustules. The best thing that you can do for your skin and your overall health is to stop smoking. Quitting cold-turkey is not always possible for everyone, and I always tell my patients that even taking baby steps can be helpful. Talk to your doctor if you need pointers on how to start the process.
2. Avoid manual exfoliation or “popping”.
The urge to self-treat your skin can be very tempting, but please don’t! While pustular psoriasis is not an infection, the high-traffic areas of your hands and feet can be hot beds for bacteria. Opening your skin can disrupt its natural barrier and clear the way for an infection.
3. Moisturize.
Help maintain your skin’s barrier with strict daily moisturizing. Choose a moisturizer with minimal irritants (e.g. fragrance or dye) and with a higher oil content. I recommend reaching for “ointments” and “creams”, rather than “lotions.” The oil-based ointments and creams will be more effective than the water-based lotions. The best time for application is after bathing or hand washing, when absorption is optimum.
4. Seek professional treatment.
I am all about easy, no-fuss treatments, but unfortunately, over the counter remedies rarely improve pustular psoriasis. Over the counter topical salicylic acid, urea, or hydrocortisone are almost always at potencies that are too low to yield any real benefit. Save room in your medicine cabinet for more heavy-hitting prescription remedies. Prescription treatments can work by targeting the inflammation that causes psoriasis, or by stimulating the regeneration or turnover of your skin.
5. Don’t ignore your joint pain.
Not all joint pain is related to psoriasis, but having psoriasis does put you at risk for a specific type of arthritis called psoriatic arthritis. This type of arthritis can be debilitating and progressive, so please make sure you discuss your symptoms with a rheumatologist or a dermatologist. Taking early action can make all the difference in the health of your joints.
6. Take a second look at your overall health.
Psoriasis has been shown to put you at an increased risk of other medical problems, such as heart disease, high cholesterol, obesity and diabetes. Recognizing this association gives you the power to take early control of your health. Talk to your doctor about any recommended medical screenings or evaluations.
Partner with a dermatologist to manage your pustular psoriasis
Managing palmar-plantar pustular psoriasis does not have to be a solo activity. Wading through the wealth of information available can be intimidating, but your dermatologist can help you navigate.