- Dr. Mark Abdelmalek
- May 13, 2022
- 1:12 pm
Skin cancer is the most common cancer. Every year more people receive a diagnosis of skin cancer than all other cancers combined.
According to the Skin Cancer Foundation, about 1 in 5 Americans will develop skin cancer in their lifetime. The vast majority of skin cancers are a result of chronic and excessive sun exposure, specifically the ultraviolet rays from the sun.
About 90% of all skin cancers are associated with ultraviolet light exposure. Most of the ultraviolet light exposure we get is from the sun, but tanning beds are an especially dangerous source of high-intensity ultraviolet light as well.
In this article we cover the most common types of skin cancer, how to identify them, and ways to prevent and treat them.
What is skin cancer and what are the most common types?
Skin cancer is an uncontrolled growth of abnormal skin cells. Skin cancer starts after the skin cell’s DNA is damaged, most often caused by harmful ultraviolet light from the sun or tanning beds. This DNA damage results in mutations of the skin cells. Once that happens, the skin cells begin to grow in an uncontrolled manner, sometimes with rapid growth. This unchecked growth is what ends up being a malignant skin cancer spot.
The three most common forms of skin cancer we see are basal cell carcinoma (BCC), squamous cell carcinoma (SCC), and melanoma.
Basal Cell Carcinoma Skin Cancer
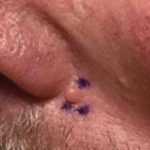
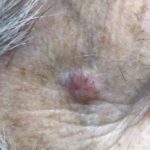
Basal cell carcinoma is the most common type of skin cancer. Fortunately, it is also the least dangerous and has the lowest chance of spreading to other parts of the body.
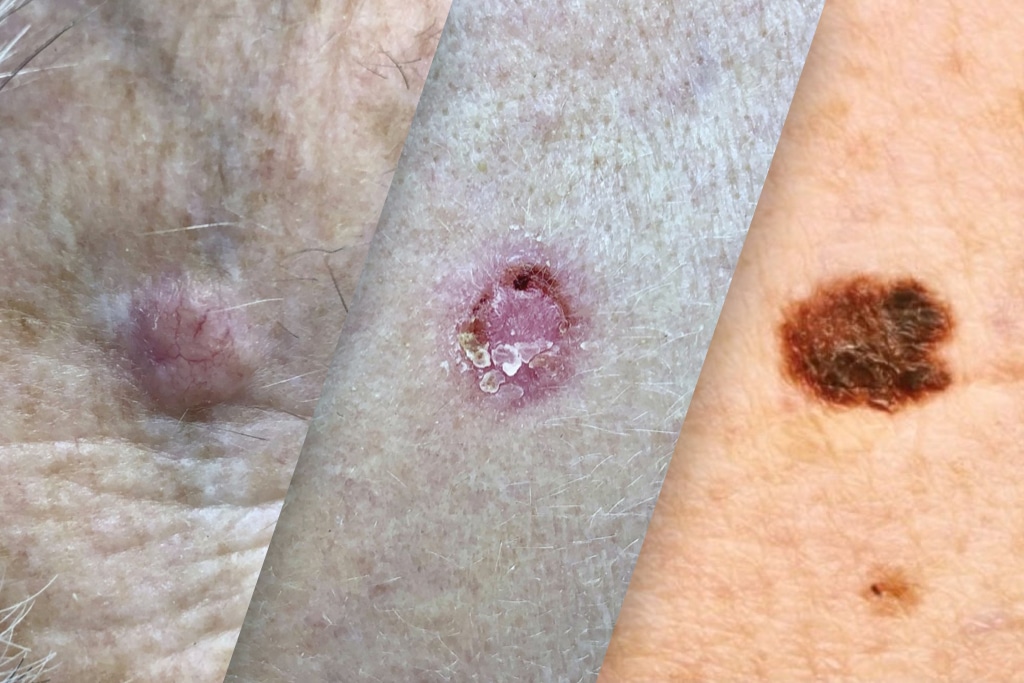
Basal cell carcinomas usually look like a sore that won’t heal or a pimple-like spot that won’t go away. Usually they grow on sun-exposed skin. Often they are shiny, pink, or pearly in appearance, but sometimes they do have a brown hue to them.
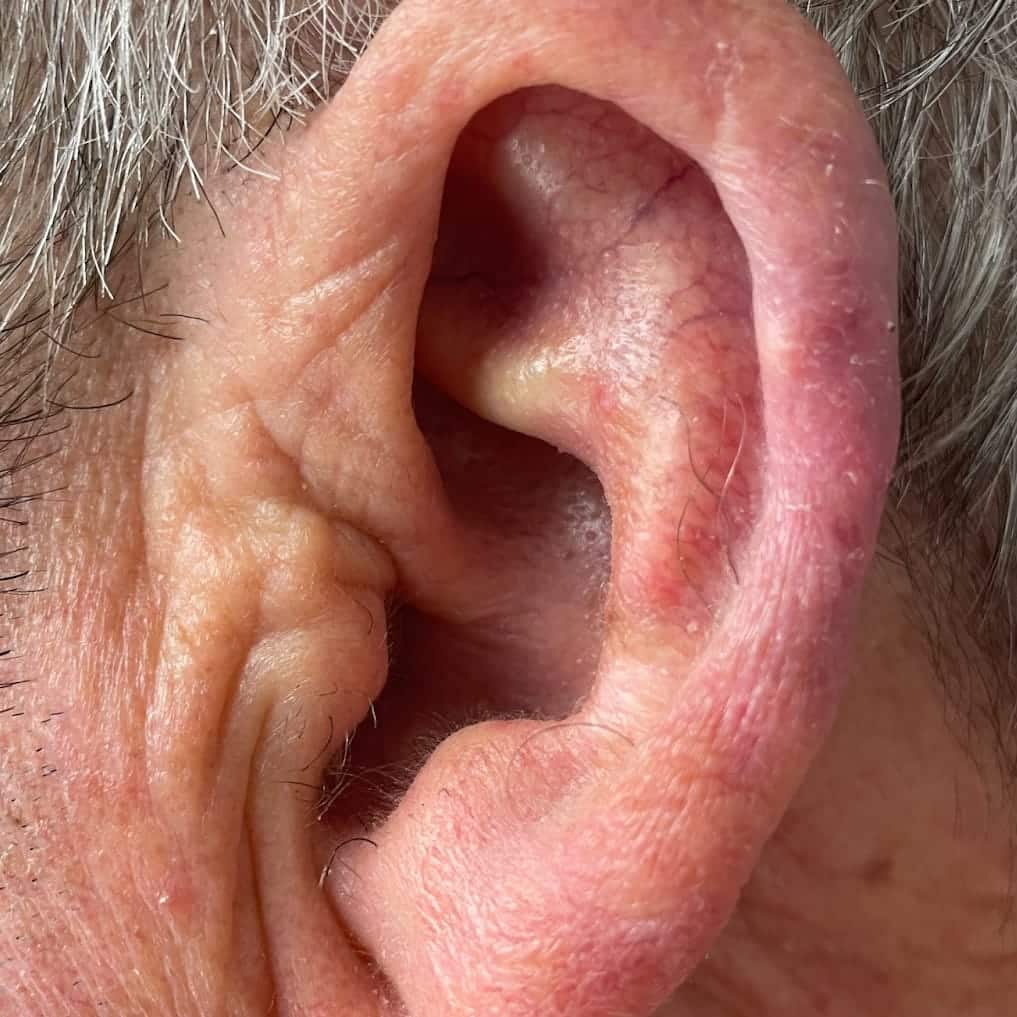
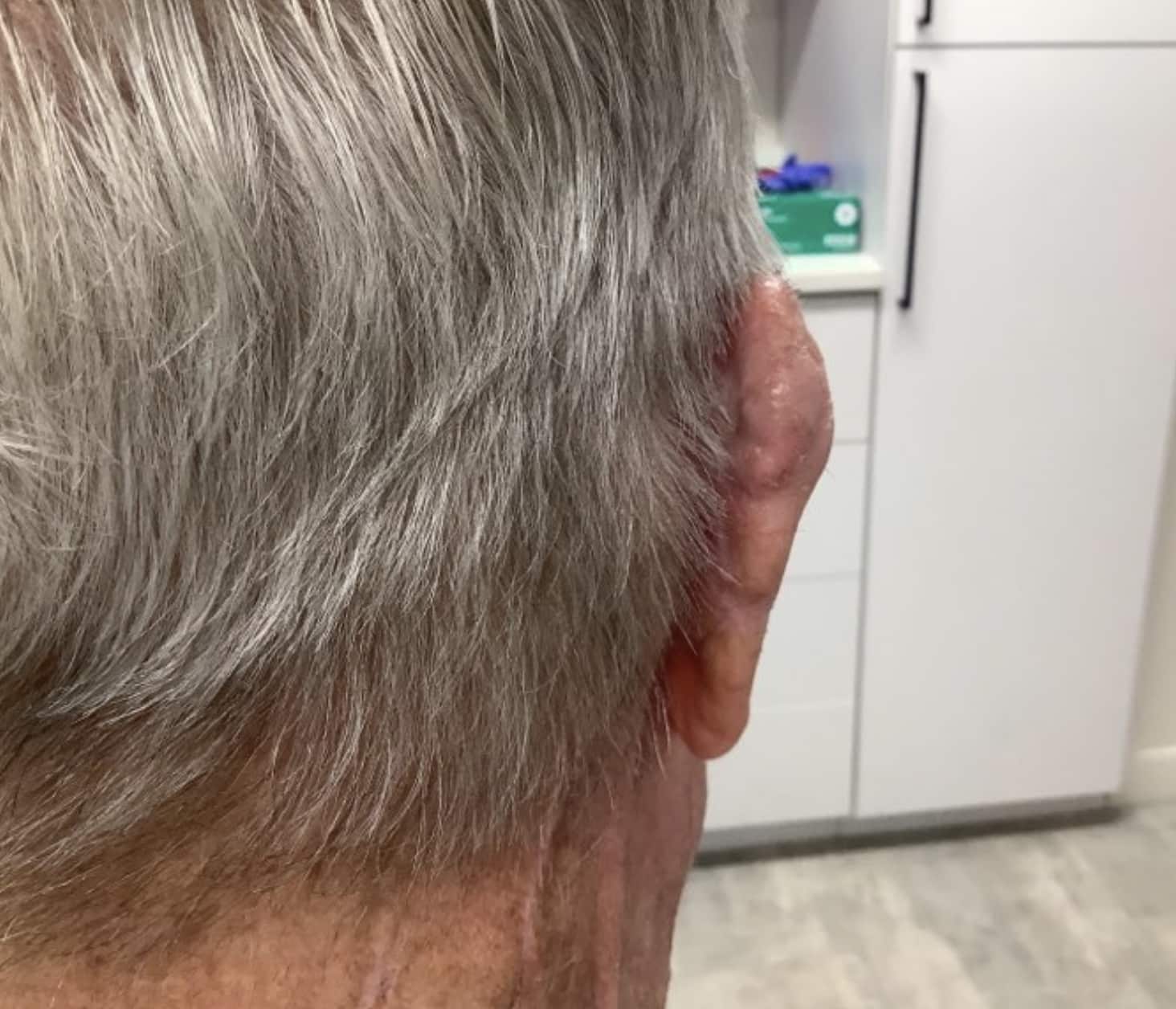
Basal cell carcinomas only very rarely spread to other areas of the body. This is not usually a concern if a basal cell is spotted, diagnosed, and treated early. However, basal cell carcinomas can be locally invasive and can extend deep into the skin, especially on the nose and ears. The longer you wait to have a basal cell treated, the more difficult it becomes to manage. Fortunately, Mohs surgery offers a very high cure rate. Dr. Mark Abdelmalek is a board-certified and fellowship-trained Mohs surgeon and Dermatology of Philadelphia provides the highest-level of care for Mohs surgery and cancer reconstruction.
Squamous Cell Carcinoma Cancer
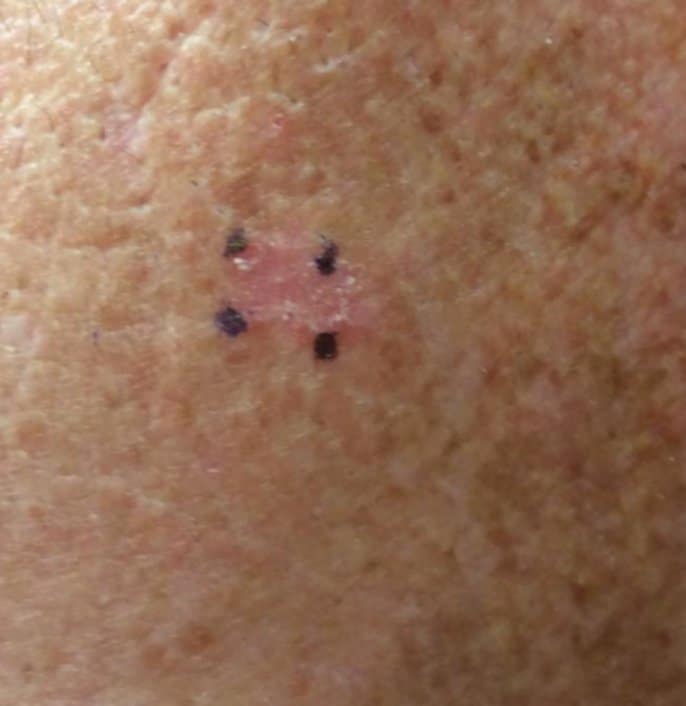
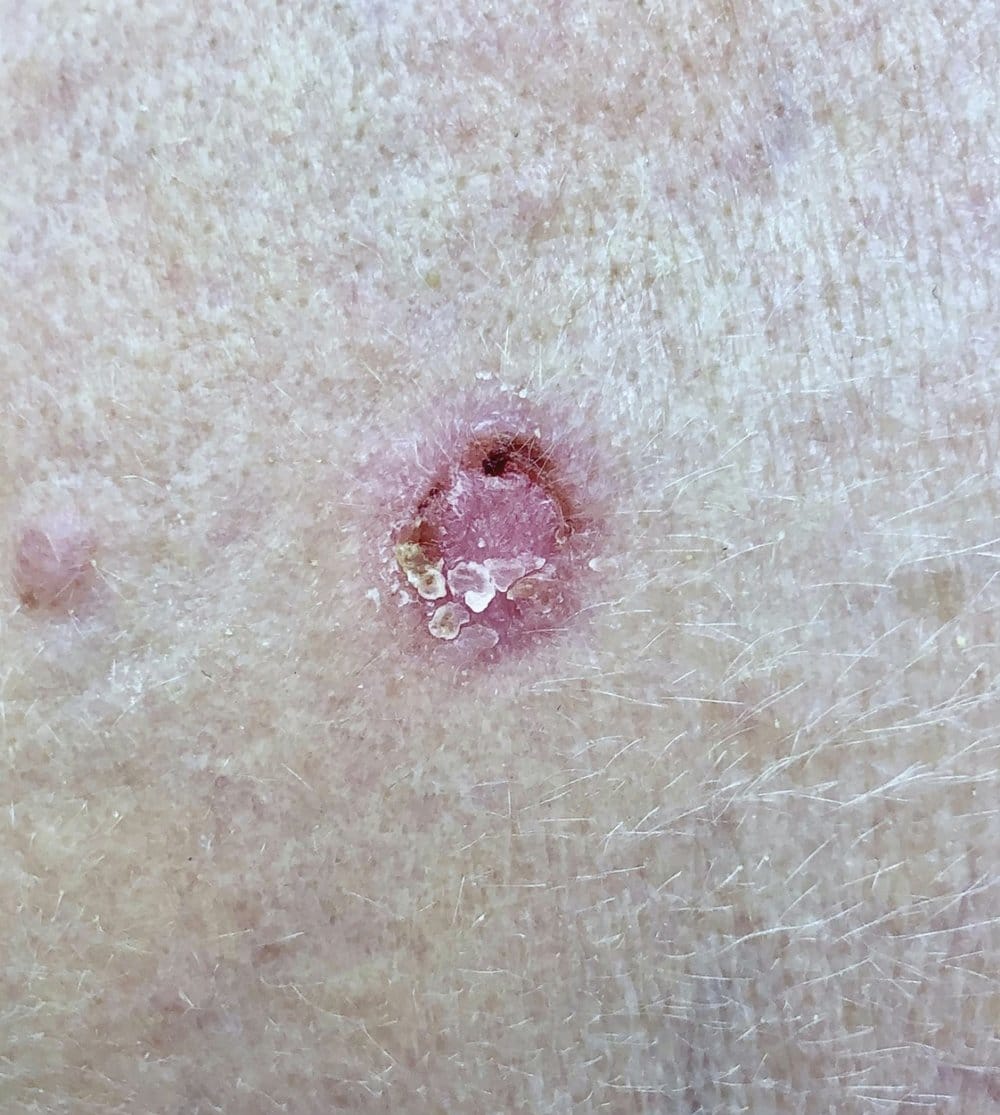
Squamous cell carcinoma is the 2nd most common type of skin cancer. Fortunately, most squamous cell carcinomas, if caught early, have a high cure rate. Squamous cell carcinoma usually arises in sun-exposed skin. The spots usually are rough, pink or red, scaly and sometimes look like a sore. They can be thick or raised.
Mohs micrographic surgery offers the highest cure rate for most squamous cell carcinomas. It is important to treat squamous cell carcinomas promptly. If left untreated, squamous cell carcinomas have the potential to spread to other parts of the body. According to the Skin Cancer Foundation, nearly 15,000 Americans die each year from squamous cell carcinoma.
Melanoma
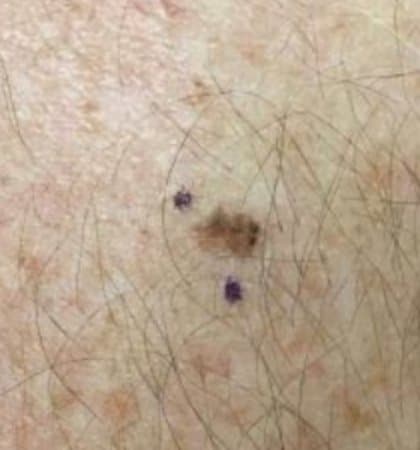
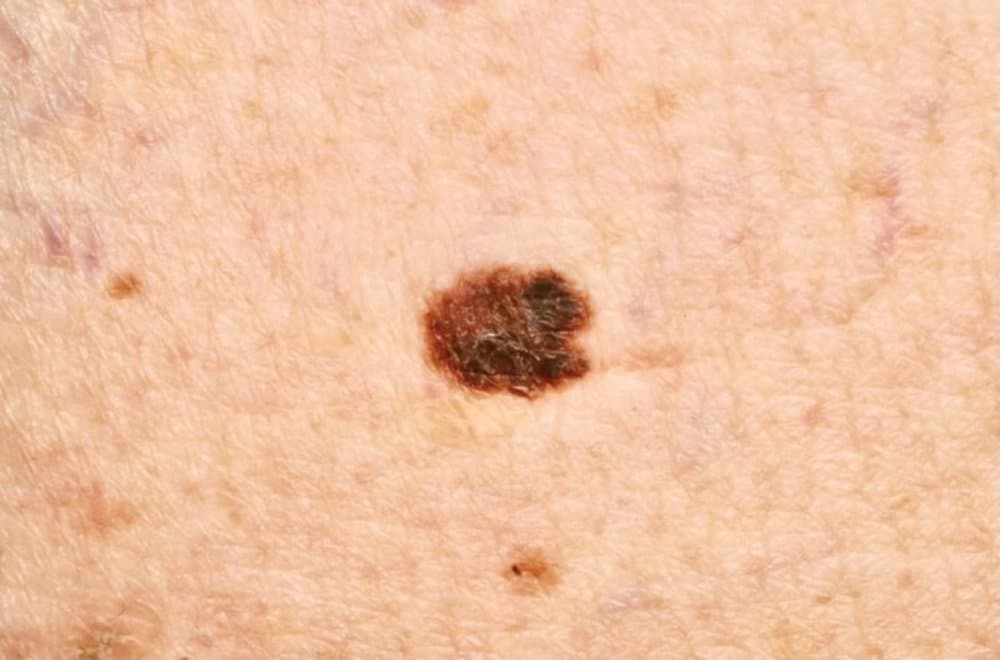
Malignant melanoma is a less common, but more serious type of skin cancer. It is an abnormal growth of “melanocytes,” which are the cells in our skin responsible for skin tone or color. Melanoma is a more dangerous form of skin cancer because it has the potential to spread to other parts of the body. But fortunately, melanoma is usually curable when detected, biopsied, and treated early. There have also been many advances in the treatment of later stage melanomas over the last five to ten years. Early detection, however, remains a very important goal in managing melanomas.
Melanoma is usually a new, dark, or changing brown lesion. However, the lesions are not always brown and are not always very obvious. According to the Skin Cancer Foundation, 20-30% of melanomas arise in existing moles. The more common scenario is a new brown spot on previously normal skin. It is for this reason that we ask patients to point out any new or changing moles they may notice.
With routine skin cancer surveillance there is a higher chance that if a melanoma is found, it is picked up early. And that matters because according to the Skin Cancer Foundation, “the estimated five-year survival rate for patients whose melanoma is detected early is about 99 percent. The survival rate falls to 66 percent when the disease reaches the lymph nodes and 27 percent when the disease metastasizes to distant organs.”
How can you lower your chances of getting different types of skin cancer?
The best and most important change you can make to lower your risk of getting any type of skin cancer is to protect your skin from the sun. Starting with:
- Wearing sunscreen everyday. Apply sunscreen everyday and make it a part of your routine. Regular and daily use of sunscreen of SPF 15-30 can lower your risk of getting skin cancer. Studies have shown that regular use of SPF 15 can reduce your risk of squamous cell carcinoma by about 40% and can lower your risk of melanoma by about 50%. Don’t forget to reapply sunscreen every few hours when outside and especially after swimming and other water activities.
- UV protective clothing and hats. UPF 50 is the number to look for. Wide-brim hats are a great way to protect your face, ears, and neck.
- Seek shade. Seek shady areas, especially during the peak sun hours between 10 AM and 2 PM.
- Wear sunglasses when outside!
What kind of sunscreens are best to protect against skin cancer?
The best sunscreen is the sunscreen you will use! Ideally everyone of all skin types should be applying a sunscreen on their face every morning with an SPF of at least 15. It doesn’t hurt to bump this number up to SPF 30 in the spring and summer months when we are outside more.
When selecting a sunscreen choose sunblocks that are labeled “broad spectrum” which indicates that the product has been shown to block both UVA and UVB rays.
When outside, at the pool, beach, or when doing water activities, find a water-resistant sunblock that you like with an SPF of at least 30.
There isn’t much benefit to using sunscreens with SPF higher than 50. Most of the sun’s rays are blocked by SPF 45-50 and adding higher SPFs (75-100) usually isn’t doing anything except costing you more!
A general rule of thumb is to apply two tablespoons of sunblock to your entire body. It’s best to do this about 30 minutes before you go outside. And as much as it is unpleasant, reapplying is very important, especially every few hours and after excessive sweating, swimming, or other water activities.
What a skin biopsy to check for skin cancer looks like?
This video is what a shave biopsy looks like. The spot was identified by the dermatologist as a possible basal cell carcinoma.
After the biopsy, the piece of skin was sent to the lab to be evaluated by a dermatopathologist. They reported back that this spot was indeed a basal cell carcinoma.
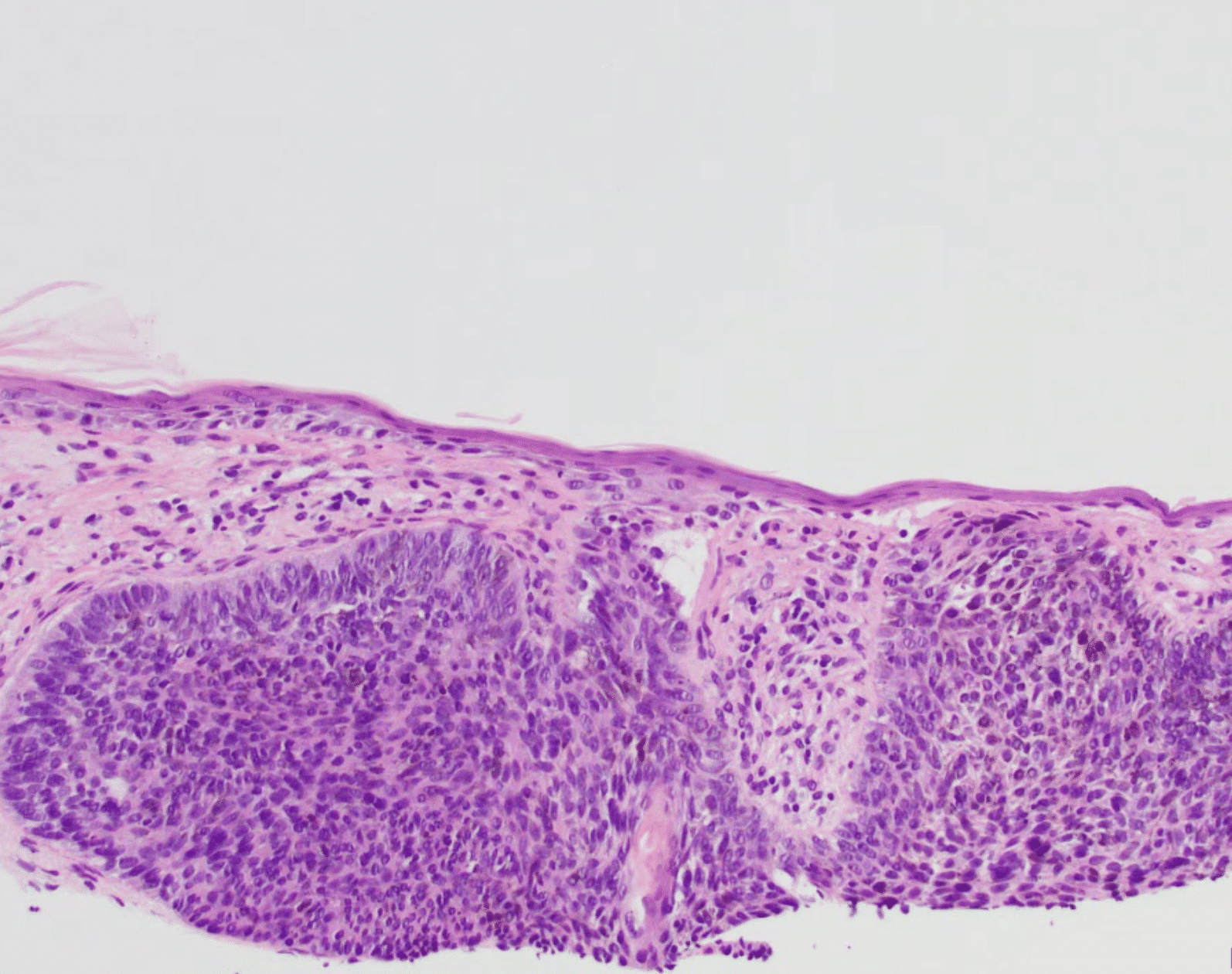
The below image shows what basal cell carcinoma looks like under the microscope. The skin cancer cells are the more purple cells in this picture. The cells are larger than normal cells and have an unorganized, crowded and abnormal growth pattern.
What to Look for: Signs of Skin Cancer
Skin cancers aren’t always obvious. They can be subtle changes, especially early on.
The most important thing to do is look at your skin in the first place. If you notice anything NEW, CHANGING, OR UNUSUAL, have it checked out by your dermatologist.
A few specific things to look for:
- A spot that is increasing in size
- A pearly, shiny, or transparent spot. Basal cell carcinomas often look like this.
- A red, scaling, or rough spot. Squamous cell carcinomas often have these features.
- A dark brown, black, red and brown, or oddly shaped brown spot with white/grey spots. Melanomas can have some of these features.
- A sore that won’t go away or a spot that is easily traumatized. These can be skin cancers. Often people think they hurt themselves or are clumsy and keep injuring themselves and dismiss spots like this. If you have a spot that is frequently looking like a cut, have it checked out. Especially if is a sore that hasn’t healed in 2-3 weeks.
ABCDEs of Melanoma
The ABCDEs of melanoma is a simple tool we often use to help patients identify spots they should bring to our attention.
A- Asymmetry. If you divide your mole in half, we want each half of the mole to look the same. If it doesn’t, let us know.
B- Border. We want moles to have a nice, regular, clean border. If the border is irregular, please let us know.
C- Color. We want moles that are a single uniform color, usually a shade of light brown. If your mole has multiple colors or is very dark in color, that is a mole that should be evaluated.
D- Diameter. We want moles to be smaller than 6 mm, or the size of a pencil eraser.
E- Evolution. This feature, perhaps more than any other, may be the most important of all. If your mole is changing or “evolving” in any way, please have that mole evaluated. Moles should not be changing.
The Ugly Duckling Sign
If you have a spot that stands out and doesn’t look like your other moles or skin spots, have that “ugly duckling” spot evaluated by a dermatologist.
How often should you have a skin evaluation by a dermatologist?
Dermatology of Philadelphia and the Skin Cancer Foundation recommend everyone see a board-certified dermatologist at least annually for a complete skin examination.
For those with non-melanoma skin cancer, we recommend an evaluation every 6 months. For those with melanoma, sometimes we ask patients to come in more often for continued skin cancer surveillance.
But don’t wait for us to look. Please examine your skin regularly as well. There is no exact frequency, but a good rule of thumb is to look at your skin the first day of every season. If you look at your skin too often, you may not notice a change. In the age of selfies and smartphones, taking a picture of a spot yourself and looking at it again in a few weeks is a good way to tell if a lesion is changing.
How is skin cancer treated?
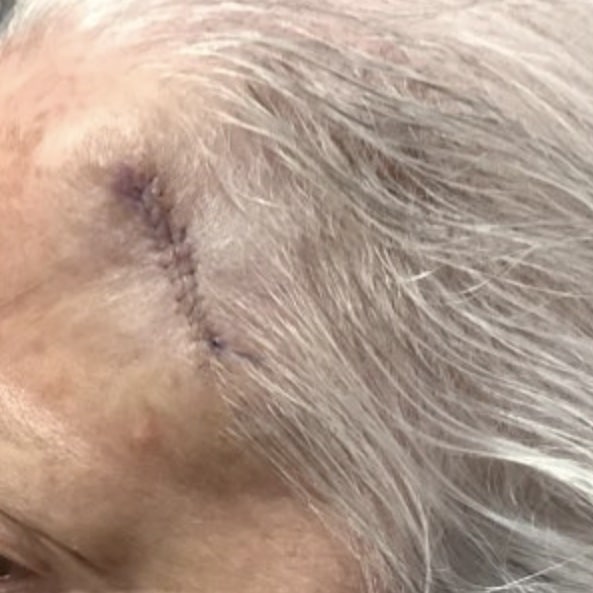
Mohs surgery is the gold standard for skin cancer treatment. Learn more about Mohs surgery with our complete Mohs surgery guide here.
For certain skin cancers and high-risk locations, Mohs surgery often offers the highest cure rate. There are, however, other ways to treat skin cancer including excisional surgery, destruction, medical management, and photodynamic therapy.